The Potentially Curable Cancer
During 2001, an estimated 135,400 Americans were diagnosed with colorectal cancer (commonly referred to as “colon cancer”) and 56,700 died from the disease. Colon cancer ranks as the third most commonly diagnosed cancer in American men and women, and the second leading cause of cancer deaths. While other cancers may be more commonly diagnosed and more frequently discussed in the media, colon cancer is actually more deadly than most. In fact, more people die from colon cancer than breast cancer or prostate cancer every year.
If detected and treated at an early stage, colon cancer has a five-year survival rate of approximately 90%. Sadly, less than 40% of cases are detected at this early, most treatable stage. Why? Many reasons. According to a recent Roper Starch survey, only 19% of adults between the ages of 50 and 74 (who have not been diagnosed with colon cancer) recognize the disease as a serious threat. Sometimes people don’t get tested because they are embarrassed to talk about this part of their body, or they fear the tests may be uncomfortable, or they simply don’t know how crucial testing is.
A common misperception is that only men get colon cancer. But colon cancer is not a “man’s disease”; in fact, more women than men get colon cancer. It is critical that everyone – women and men – talk to their doctors about when they should get tested, especially people 50 or older or those with a higher risk for the disease. Doctors can find growths on the inner wall of the colon known as polyps and remove them before they become cancerous – preventing colon cancer before it even starts! And remember: Even if the cancer is already present, there is a much greater chance of curing it if it’s found in an early stage.
Precautions You Can Take
Most people diagnosed with colon cancer are 50 or older, but personal risk for the disease varies. African Americans have a higher risk for the disease. And a family history of colon cancer or colorectal syndrome (such as Gardner’s syndrome) can increase your risk. So can a personal history of inflammatory bowel disease. These are genetic and medical factors you can’t change; but the good news is that there are things you can do to reduce your chances of getting colon cancer:
Eat right for life! Eat mostly fruits and vegetables; keep your fat intake to less than 30% of your total calories; avoid foods high in cholesterol; and limit alcohol intake.
Watch your weight. Studies show that maintaining a healthful body weight decreases cancer risk. And since we all know staying physically active is good for us, this is one more reason to get moving.
If you smoke or use other tobacco products, quit. A higher risk for colon cancer makes this habit even more dangerous.
Screening Options
The early stages of colon cancer are often symptom-free. So getting regular exams can literally save your life. For all men and women, the American Cancer Society recommends one of these five testing options beginning at age 50:
Yearly fecal occult blood test (FOBT)
Flexible sigmoidoscopy every five years
Yearly FOBT and flexible sigmoidoscopy every five years (preferred over either option alone)
Double contrast barium enema every five years
Colonoscopy every 10 years
Discuss these options with your doctor to determine the best testing method for you. Your doctor can also help you make an informed decision on whether your personal risk warrants testing before age 50. Discussing your bodily functions might not be the easiest thing to do, but don’t be embarrassed. Health care professionals are specially trained to answer your questions honestly and without judgment.
Remember, this potentially deadly disease strikes both men and women, but it is PREVENTABLE (and highly curable if found in an early stage). So – Get the test. Get the polyp. Get the cure.
What is Ovarian Cancer?
Ovarian cancer is a cancer that affects the ovaries, a pair of almond shaped glands that lie on each side of the uterus, located in the pelvis. These female reproductive organs have two functions: they store eggs and secrete the hormones (chemicals that control the way certain cells or organs function) which regulate pregnancy and menstruation. Ovarian cancer occurs when cells in the ovary become abnormal and divide without control or order. Cancer cells can invade and destroy the tissue around them. They can also break away from the tumor and spread to other parts of the body.
Symptoms
• Vague but persistent gastrointestinal complaints such as gas, nausea, and indigestion
• Pelvic and/or abdominal swelling and/or pain; bloating and/or a feeling of fullness
• Unexplained change in bowel habits
• Unexplained weight gain or loss
• Frequency and/or urgency of urination
• New and unexplained abnormal postmenopausal bleeding Risk Factors
• Increasing age with the highest occurrence in women over age 50
• Family history or personal history of ovarian, breast, endometrial or colon cancer
• No pregnancies, infertility (uninterrupted ovulation)
• Presence of BRCA1 or BRCA2 gene mutations Prevention and Detection
• The use of oral contraceptives for more than five years can reduce your risk by 50%
• Multiple pregnancies and breast feeding can reduce the risk
• Removal of the ovaries (prophylactic oopherectomy or tubal ligation may reduce but not eliminate individual risk)
The single most effective way a woman can protect herself against ovarian cancer is to become educated about it so she can make informed decisions about her health. Listen to your body; do not ignore symptoms.
Fiber may Prevent Colon Cancer
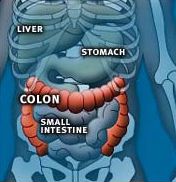 New research has revived the notion that a high-fiber diet may protect against colon cancer. Long-standing recommendations for high-fiber diets have taken a hit over the last few years after a handful of carefully conducted studies failed to find a benefit. But experts say two major studies published this week in The Lancet medical journal — one on Americans and the other on Europeans — indicate previous research may not have examined a broad enough range of fiber consumption or a wide enough variety of fiber sources to show an effect.
New research has revived the notion that a high-fiber diet may protect against colon cancer. Long-standing recommendations for high-fiber diets have taken a hit over the last few years after a handful of carefully conducted studies failed to find a benefit. But experts say two major studies published this week in The Lancet medical journal — one on Americans and the other on Europeans — indicate previous research may not have examined a broad enough range of fiber consumption or a wide enough variety of fiber sources to show an effect.
The new studies indicate fiber intake needs to be about 30 grams a day to protect against colon cancer. “THESE TWO new findings show that the fiber hypothesis is still alive,” said the leader of the American study, Ulrike Peters of the National Cancer Institute. Figuring out the relationship between nutrition and disease has always proved difficult, but experts say fiber is particularly complicated because there are various types and they all could act differently. Fiber is found in fruits, vegetables and whole grains. Americans eat about 16 grams a day, while Europeans eat about 22 grams. The new studies indicate fiber intake needs to be about 30 grams a day to protect against colon cancer. There are 2 grams of fiber in a slice of whole meal bread. A banana has 3 grams and an apple has 3.5 grams, the same as a cup of brown rice. Some super-high fiber breakfast cereals have as much as 14 grams per half cup.
DECREASED RISK OF GROWTHS
In the American study, investigators compared the daily fiber intake of 3,600 people who had precancerous growths in the colon with that of around 34,000 people who did not. They were divided into five groups, according to how much fiber they ate. The average roughage intake in the lowest group was 12 grams a day, while in the highest group it was 36 grams a day. People who ate the most fiber had a 27 percent lower risk of precancerous growths than those who ate the least. In the European study, the largest one ever conducted on nutrition and cancer, scientists examined the link in more than 500,000 people in 10 countries. As in the American study, questionnaires separated the people into five groups, according to fiber intake. Following them for an average of four years, 1,065 of them had developed colorectal cancer. Those who ate the most fiber, about 35 grams a day, had about a 40 percent lower risk of colorectal cancer compared with those who ate the least, about 15 grams a day, the study found. “In the top quintile (group) they were eating 15 grams of cereal fiber, which is equivalent to five or six slices of whole meal bread, plus they were eating seven portions of fruit and vegetables a day, which is basically the Mediterranean levels,” said the study’s leader, Sheila Bingham, head of the diet and cancer group at Cambridge University’s human nutrition unit.
AN AGE-OLD DEBATE
Discussions about the link between fiber and bowel health — or, at least the relative merits of white and brown bread — date back to antiquity. In a twist on modern thought, Hippocrates, who lived in the 5th century B.C., believed white bread was more nutritious because it creates less feces than brown bread. Scientists now believe the extra feces is a benefit. The contemporary theory that fiber wards off colon cancer began in the 1970s, when a British doctor, Denis Burkitt, noted that poor people in Africa produce more feces than Westerners and get much less colon cancer. One obvious difference between the two groups was that Africans consumed more fiber. Scientists believe that fiber dilutes and absorbs cancer-causing agents and makes them flow more quickly through the body. Researchers have also theorized that a high-fiber diet makes protective changes to cells or curtails bile acids that irritate the intestinal lining and promote growths. The first big dent in the theory came in 1999 from a study that tracked the eating habits of 88,757 American nurses for 16 years. The risk of colon cancer was the same, regardless of how much fiber the women were eating. Then in 2000, two studies which used a different method also came up negative. They put people on different diets and counted precancerous growths in their colons for up to four years. There was no apparent effect from high-fiber diets or supplements. One major difference between the former and current studies is that the new ones examine more diverse populations who eat different types of fiber and in hugely varying amounts. However, Andy Ness, a lecturer in epidemiology at Bristol University in England, who was not connected with either study, said the latest research is not the last word. “Across Europe, there is an amazing variation in risks of cancer. There is also a huge variation in diet, so across these cultures you can get this breadth of intake. However, what you might be picking up across this range of diet is a range of cultures. It’s possible it’s something else that goes with that pattern of diet,” he said.
About 135,400 new cases of colorectal cancer will be diagnosed in the United States this year and 56,700 patients will die. But early detection can be a lifesaver.
Beginning at age 50, the American Cancer Society recommends that both men and women at average risk should have one of the following screening regimens:
- Fecal occult blood test every year*
- Flexible sigmoidoscopy every five years*
- Yearly fecal occult blood test plus flexible sigmoidoscopy every five years* (Of the first three options, ACS prefers this one)
- Double contrast barium enema every five years*
- Colonoscopy every 10 years*
*A digital rectal exam should be done at the same time as sigmoidoscopy, colonoscopy or double-contrast barium enema. People considered “high risk” should undergo more frequent screening of the entire colon, usually with colonoscopy, beginning at a younger age. Talk to your doctor about the schedule best for you
People considered at “high risk” for colorectal cancer are those with:
- A strong family history of colorectal cancer or polyps
- A family history of familial adenomatous polyposis or hereditary nonpolyposis colorectal cancer (HNPCC)
- A personal history of colorectal cancer or adenomatous polyps
- A personal history of inflammatory bowel disease (ulcerative colitis or Crohn’s disease)
Here are some of the techniques used to help detect the disease early:
Fecal Occult Blood Test (FOBT): This is a stool test that looks for microscopic amounts of fecal blood that cannot be seen on visual inspection. This test, also referred to as the “stool guaiac,” is performed by placing a small amount of stool on a specially treated card that is developed in the doctor’s office or lab. If the card turns blue, the test is positive. A fecal blood test costs just $10 to $25.
Double contrast barium enema: This radiographic procedure uses a material called barium that “lights up” on X-rays. Barium and air are delivered to the colon by means of a tube that is inserted into the rectum. This is solely a diagnostic procedure, done without sedation.
Flexible sigmoidoscopy: A flexible tube with a light and camera on the end (called an endoscope) is inserted into the rectum and lower third of the colon. If identified, polyps can be removed at the same time and biopsied. This procedure is usually done without sedation and lasts about five to 15 minutes. Sigmoidoscopy, which costs $100 to $200, uses a less-sophisticated viewing tube than colonoscopy and cannot probe the colon’s top two-thirds, where growths become more common, dangerous and hard to detect with age.
Colonoscopy: This procedure is similar to the flexible sigmoidoscopy except that the entire colon is visualized. Sedation is used to make patients comfortable. If identified, polyps can be removed at the same time and biopsied. This procedure takes 20 to 45 minutes. Costing at least $1,000, colonoscopy is about 95 percent accurate and is currently only recommended every 10 years, starting around age 60 for people with no family history of colon cancer.
Pancreatic Cancer: A Stubborn Foe
- Because the organ is located deep inside the abdomen, disease symptoms can be tough to detect.
The type of cancer called neuroendocrine pancreas tumor — afflicts only some 1,000 people a year in the United States, compared to the 40,000 cases of the far more lethal “traditional” pancreatic cancer, the fourth leading cause of cancer death of Americans.
Some 50 percent to 60 percent of people with neuroendocrine tumors will be alive five years after their diagnosis, vs. only 5 percent to 10 percent of patients with traditional pancreatic cancer, said Dr. Daniel Labow, chief of surgical oncology at Mount Sinai Hospital in New York City.
Neuroendocrine tumors often start in the pancreas but more commonly appear first in the small intestine and, less commonly, in the appendix, stomach and rectum, Labow said.
The pancreas is situated deep inside the abdomen, between the stomach and the spine. It has two main functions: an exocrine function that helps with digestion and an endocrine function that regulates blood sugar, according to Columbia University’s College of Physicians and Surgeons.
Because the pancreas is positioned deep inside the body, it’s often difficult to diagnose tumors early because they have yet to interfere with the function of nearby organs such as the stomach, liver or gallbladder, according to Johns Hopkins University.
Neuroendocrine tumors originate in cells that make hormones, triggering hormone overproduction. The mainstay of treatment is surgery, and sometimes injections to block the hormones. Traditional chemotherapy is rarely effective, Labow said.
Liver transplants are also often necessary and, in the past year, the U.S. Food and Drug Administration approved two new drugs for neuroendocrine tumors — sunitinib and everolimus.
While Jobs lived eight years with his diagnosis, the average survival time for advanced pancreatic cancer is much worse, roughly only eight or nine months, said Dr. Maged Rizk, a gastroenterologist with the Cleveland Clinic.
Because traditional pancreatic tumors tend to be diagnosed later, rather than sooner, that’s a big reason why they’re so deadly, Rizk added.
“If the tumor is in the head of the pancreas, then there’s a high chance that it will cause obstruction in the bile duct, the patient will turn yellow and have an infection so we pick it up earlier than if it’s in the tail, where the chance of it causing symptoms is less,” Rizk explained.
Also, he said, the pancreas pushes up against blood vessels and lymph nodes, making it easier for cancer cells to invade these systems and travel throughout the body.
On the other hand, neuroendocrine tumors are distressing because they tend to afflict people in their 30s and 40s (Jobs was diagnosed in his late 40s), whereas the average age at diagnosis for pancreatic cancer is 60, Labow said.
Risk factors for neuroendocrine tumors are largely unknown. Risk factors for pancreatic cancer include not only age, but cigarette smoking, obesity, diabetes and race — blacks are more likely to develop the disease than whites.
THURSDAY, Oct. 6 (HealthDay News) -- By Amanda Gardner, HealthDay Reporter
Drinking More Fluids Could Lower Men’s Bladder Cancer Risk
The association was not as strong in older males who typically drank less water, study finds
Men who drink plenty of low-sugar fluids may reduce their risk for bladder cancer, new research suggests.
Although the reason for the association between fluid intake and protection against cancer remains unknown, researchers theorize the fluids may flush out potential cancer-causing agents before they have a chance to cause any damage.
In conducting the study, Jiachen Zhou, a doctoral candidate in epidemiology at Brown University, and colleagues evaluated the fluid intake of nearly 48,000 men who were part of a long-term study. The men, who were aged 40 to 75 when they enrolled in the study in 1986, answered a questionnaire about their fluid intake every four years for more than two decades.
The investigators found that the men with a high daily fluid intake, or those who drank more than 10 cups (2,531 milliliters) per day, had a 24 percent reduced risk for bladder cancer. The study authors concluded that doctors should tell their patients to drink plenty of low-sugar fluids.
Although this link between fluid intake and bladder cancer risk was discovered 10 years ago, the association, the study found, was stronger among younger men. This could be due to the fact that the men drank less as they aged, particularly water, the researchers pointed out in a news release from the American Association for Cancer Research.
The study findings — which revealed an association between fluid consumption and reduced cancer risk, but not a cause-and-effect — were slated for presentation Oct. 24 at the AACR International Conference on Frontiers in Cancer Prevention Research, in Boston. Research presented at medical meetings should be viewed as preliminary until published in a peer-reviewed journal.
(HealthDay News) -- American Association for Cancer Research, news release, Oct. 2011
Helpful Info..
What Causes Cancer?
Cancer is a complex group of diseases with many possible causes. In this section you can learn more about the known causes of cancer, including genetic factors; lifestyle factors such as tobacco use, diet, and physical activity; certain types of infections; and environmental exposures to different types of chemicals and radiation.
http://www.cancer.org/cancer/cancercauses
